Inflammatory Bowel Disease (IBD), characterized by repeated episodes of inflammation, can make it difficult to maintain a diverse and nutrient-rich diet because of the symptoms. People may avoid eating due to symptoms such as nausea, abdominal pain, vomiting and diarrhea during disease inflammatory activity. With IBD, including Crohn’s Disease and Ulcerative Colitis, there is constant worry about food triggers and the risk of various nutritional deficiencies due to decreased food intake, disruption of food absorption, increased energy expenditure, and/or increased bone or muscle loss.
People with IBD often experience weight loss and reduced muscle mass. The primary causes of reduced muscle mass are inflammation, decreased physical activity, and steroid medications used to treat IBD.
Low bone mass is also common with IBD. The cause is due to many factors, including steroids used in IBD treatment.
IBD’s location and degree of involvement in the intestines influence the risk of specific nutrient deficiencies. Involvement of the distal segment of the small intestine may lead to deficiencies of vitamin B12 or fat-soluble vitamins. Iron and calcium absorption are affected with involvement of the proximal small intestine. Also, diffuse small bowel disease with profuse diarrhea may cause zinc deficiency. And, severe colon disease may lead to ongoing blood loss and iron deficiency.
Bile juice breaks down the fat, and is reabsorbed in the distal segment of small intestine. The absorption of fat can be affected because of bile acid deficiency, due to involvement of the distal segment of the small intestine, or resection in IBD. Deficiencies of fat-soluble vitamins (vitamins A, D, E and K) are most likely to occur in people with fat malabsorption.
Potential contributors of anemia in people with Inflammatory Bowel disease (IBD) are iron deficiency, vitamin B12 or folate deficiency, chronic inflammation, and side effects of medications – Sulfasalazine, Methotrexate, Azathioprine and 6-Mercaptopurine.
The most common micronutrient deficiencies in people with IBD are vitamin D, vitamin B12, iron, zinc and calcium. Less common deficiencies are vitamin A, vitamin E, vitamin K and folic acid.
Iron
Iron is the component of hemoglobin found in red blood cells. Iron deficiency is the most important contributor to anemia in people with IBD.
There are several mechanisms which contribute to iron deficiency in people with IBD. These include chronic intestinal bleeding, disease involving the initial part of the small intestine where iron is predominantly absorbed, and inflammation causing decrease mobilization of iron stores from the liver and spleen.
In children, iron deficiency significantly and negatively impacts quality of life, cognitive and developmental abnormalities. People with IBD are generally screened periodically by their doctor using complete blood count (CBC) tests.

Foods to consider after talking to your doctor or dietitian are:
- White beans
- Lentils
- Kidney beans
- Chickpeas
- Oysters
- Sardines
- Stewed tomatoes
- Iron fortified cereals
Your doctor may recommend iron supplements if you have iron deficiency anemia and are not getting enough iron from food sources.
Vitamin D
Vitamin D is required for healthy bones along with calcium. It is also involved in regulating the immune system, and has been investigated as a possible adjunctive therapy in IBD.
Vitamin D deficiency may be due to several factors. These include improper absorption and anorexia due to IBD, steroid medication used in treatment, diet and sun exposure.
Foods that are rich in vitamin D to consider after talking to your doctor or dietitian are:
- Sardines
- Orange juice
- Cod liver oil
- Tuna
- Salmon
- Fortified cereal
- Egg yolk
Vitamin B12
Vitamin B12 is a micronutrient that keeps nerves and red blood cells healthy. Vitamin B12 is absorbed in the small intestine.
Deficiency in vitamin B12 leads to anemia and nerve problems. The deficiency is further exacerbated in Crohn’s disease because of the involvement of small intestine. Other factors that may contribute to deficiency are resection of the distal segment of small intestine, gastritis (a condition that inflames the stomach lining), and bacterial overgrowth. Vegetarians are also at risk for developing vitamin B12 deficiency.
Food sources containing vitamin B12 include:
- Clams
- Trout
- Tuna
- Liver
- Fortified cereals
- Milk
- Beef

Zinc
Zinc helps in building the immune system and in the functioning of metabolism. It is also important for wound healing, and your sense of taste and smell. Zinc deficiency affects the skin, causing dry and scaly patches.
Diffuse diarrhea, ostomies and fistulas may contribute to the excess loss of zinc.
Zinc food sources to consider after consulting with your doctor or dietitian include:
- Crab
- Shellfish
- Oysters
- Whole grains
- Fortified grains
- Legumes
- Nuts
- Green peas
- Bran
- Poultry
Calcium
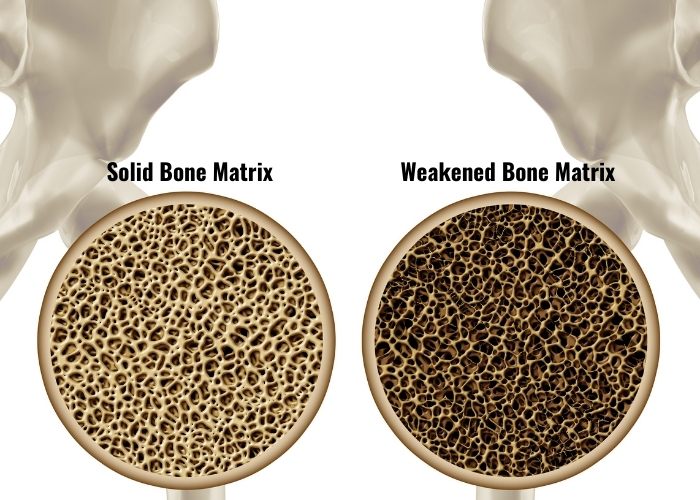
Calcium is required for healthy bones and teeth, and for regulating muscle functioning. Calcium deficiency is very common in people with IBD, even more so if you are being treated with steroids. Steroid use can lead to low bone density, making the bones weak and fragile.
Good sources of calcium in food include:
- Broccoli
- Salmon with bones
- Shrimp
- Sardines
- Dark leafy green vegetables
- Foods fortified with calcium
| Symptoms or Condition | Causes in IBD |
|---|---|
| Anemia causing fatigue, shortness of breath, irregular heartbeats | Iron deficiency, vitamin B12 and folate deficiency, chronic inflammation, medications including Sulfasalazine, Methotrexate, Azathioprine, 6-Mercaptopurine |
| Bone loss (osteoporosis) with increased risk of fractures | Chronic inflammation, steroid therapy, vitamin D and calcium insufficiency |
| Dry scaly rashes often on the face, and around the genital areas and anus Stunted growth | Zinc deficiency |
| Numbness, or tingling in the hands, legs or feet Memory loss, or difficulty thinking and reasoning (cognitive difficulties) | Vitamin B12 deficiency |
| Calcium oxalate kidney stones | Calcium deficiency |
Less common deficiencies:
Folic acid
Folic acid deficiency is uncommon in people with IBD, except in patients with specific risk factors, which include treatment with Sulfasalazine or Methotrexate.
Vitamin A
Vitamin A deficiency may occur in people with extensive small bowel involvement and/or fat malabsorption, since vitamin A is a fat-soluble vitamin.
Vitamin E
People with significant fat malabsorption, as seen in small bowel involvement, may have deficiency of vitamin E, a fat-soluble vitamin.
Vitamin K
Contributing factors may include fat malabsorption (particularly with terminal ileal disease or resection), decreased food intake due to dietary restrictions or anorexia, and/or antibiotics (which interfere with vitamin K production by intestinal bacteria).
Selenium, phosphate, copper and magnesium deficiencies can reflect generalized malnutrition and occur occasionally in patients with IBD.
Work with your doctor or dietitian, and understand the different types of nutritional support. Keeping a log of all foods and beverages you consume daily, and learning how different foods interact with the body, can help you be as healthy as possible. It is a balancing act between eating healthy and avoiding foods that worsen IBD symptoms. There is no one-size-fits-all solution when it comes to nutritional therapy with Crohn’s disease and ulcerative colitis. The use of nutrition strategies is almost always tailored for each patient.


