Learn about the process of starting a new Lupus drug from an award-winning health blogger and author living with Lupus.
There was a point in my Lupus journey where I had a major decision to make. My doctor wanted me to consider starting Methotrexate, a drug I’d hardly heard of. Over the months prior, my joint pain and swelling had become pretty unmanageable, so he thought we should try something new. I asked for a few weeks to: a) think about it, and b) give my current medication one last shot at controlling my symptoms. I was in the middle of a Prednisone taper (yet again), so it was a good time to do a bit of assessing.
Here were the questions on the table:
1) What is Methotrexate, and what would it look like if I started taking it?
2) What is my current level of disease activity? Is it something I can tolerate? Is it something I should tolerate?
3) If my current level of symptom activity is or becomes manageable, is the lifestyle I’ve adopted to keep it that way manageable?
Number One: What is Methotrexate?
The goal here was to shift my mindset to be opened-minded about starting a new drug. I can’t think of Methotrexate as “a drug I really don’t want to start”, which is the way I felt when my doctor initially brought it up. Instead, I needed to think, “Here’s a drug my doctor’s considering. What are the pros, the cons, and how will it compare to what I’m currently taking regarding side effects, symptom control, etc.?” I know – serious patient maturity required here!
But I’d done my due diligence. I’d researched the drug online. I’d asked my other doctors for input. I’d talked to my friends who were on it. I’d considered the side effects and the limitations, and mentally prepared for them as much as possible. Most importantly, I’d acknowledged that if my current medication regimen isn’t doing the job, I needed to find something that will. Sure, it was difficult to comprehend why my beloved combination of Plaquenil and Prednisone had suddenly stopped working – after all these years. And I could have continued to search for answers, or even worse, try and force my body to conform. But what would be most productive was to listen to my body and accept what it’s saying. If my disease had changed such that my medication needed to change, then that’s what I needed to do.
Number Two: Current symptom activity – is it manageable?
The only way I know how to determine how good or bad my symptoms really are is to track them. When I’m dealing with varying degrees of joint pain and swelling from morning until evening, and sometimes through the night, there’s no way I can accurately or objectively log that activity in my head. I start getting yesterday’s symptoms confused with the day before, and before you know it, I can’t remember how long it’s been since I haven’t been able to turn over in bed or fasten my clothes first thing in the morning.
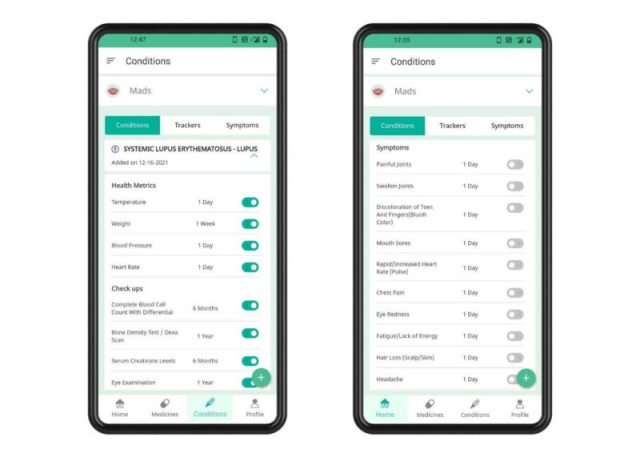

That’s where the KnowYourMeds app comes in handy. I can track joint pain, swelling, fever, fatigue, and anything else that is impacting my quality of life. I can even export a report that will show my flow of symptom activity in the form of a graph. When I was considering Methotrexate, I wasn’t interested in what factors were contributing to my flare. I just wanted to know how well my current medications were managing that flare, and how reasonable (or unreasonable) that level of management was.
The graph function in particular worked really well on the app. The visual picture of what I’d been experiencing was really coming into view. It was becoming clear that it wasn’t just steroid withdrawal I was experiencing. My symptoms were still pretty active, and I still had a few steps to go on my Prednisone taper. Pretty obvious when you see it in black and white.
Number Three: Are my lifestyle accommodations sustainable? (Aka, if the pain is tolerable, how long can I keep up the charade?)
As one runs through these kinds of questions, one always has to consider this fact: your doctor gets to weigh in on the situation, too. I could show up to my next appointment, and he may say that my kidney function isn’t good, my lungs aren’t clear, or my blood tests are out of whack. Any of those might necessitate a change in medication or treatment, which would make whatever decision I’ve come to obsolete.
I’ve upended many aspects of my life to accommodate my disease over the years. I’ve inserted naps, rearranged agendas, cancelled plans, and revised goals in order to do what I can to keep disease activity at bay. And I’ve reached a comfortable level of living well, despite those accommodations. While I know my life with lupus isn’t necessarily normal, it’s my normal. There’s a certain level of predictability that I’ve come to expect, and it works. But when I was considering this change to Methotrexate, I’d been forced to create additional workarounds throughout the day in order to stave off severe symptom activity. And the question was – how long can that go on before I conclude that those new lifestyle accommodations were abnormal? When do I decide that I’m no longer living well, despite lupus?
My dad and I were talking about how difficult it can be to figure this out. If you’re like me, you try to put a pretty positive spin on life as it is. In fact, my dad referenced a book that I’d recommended to him, “Flying Without Wings”, by Dr. Arnold Beisser. Beisser says there’s a certain “degree of denial” that’s necessary for any of us to carry on in this crazy world, given whatever our cross is to bear. And I completely agree with that. But because of that fact, I made a promise to myself years ago, once I’d recognized how permanent this whole lupus thing was going to be. I could think positively, and hope for the best. But when it came to assessing how things were really going, I needed to muster up the courage to distinguish hopes from reality. I needed to be strong enough to take a step back, and objectively evaluate how good (or bad) my disease activity was.
What did that mean? It meant I wouldn’t lie to myself. I wouldn’t pretend to be feeling great, if I really wasn’t. Nor would I lower my standards so that I could say things weren’t that bad. Of course, this promise came after years of doing just that – acting like the disease wasn’t affecting me, even though my body was saying something else. After finally learning how to embrace my disease rather than fight against it, I concluded that being honest with myself is essential for living well. It boils down to this – even if the pain is tolerable, how long can you keep up the charade?
Truth was, I couldn’t pretend that the changes I’d made over the months prior weren’t out of the ordinary. The trips we’d put off, the nights we’d stayed in, or the appointments I’d cancelled in order to try and keep that flare from progressing were not long-term solutions. Those were things I do in crisis-mode, or should I say, flare-mode. When it comes to living well as a permanent state of being – my definition includes a certain degree of painlessness, while maintaining a personally fulfilling lifestyle, whatever that looks like to me. If there’s a way, via Methotrexate, Cellcept or some other big gun medication, to achieve that personal level of comfort and fulfillment, then I say bring it.
I had too much to do and too little time to waste pretending that my joints didn’t hurt. I could plot all day long, but if at the end of that tapering period, my level of pain was unacceptable, or the workarounds were too extraordinary, then I needed to do something about it. And if my doctor had a solution, I needed to take him up on it. Considering a new drug that your doctor has proposed, or have questions about one you’re already on? Don’t forget to chat with KnowYourMeds’ in-app pharmacist. As always, I’m also happy to offer a patient perspective!


