Inflammatory Bowel Disease (IBD), which includes two chronic relapsing conditions, Ulcerative Colitis and Crohn’s Disease, affects millions of people worldwide. The reason these conditions occur is unknown, but is believed to be due to complex interactions between human genetics, environmental factors, and gut microbiota.
Having a chronic illness, such as IBD, brings a significant amount of stress. Managing and juggling domestic duties, work, relationships, and disease can be overwhelming at best. Your quality of life can be greatly affected by these simultaneous challenges.

So, exactly what is stress?
Stress is an adaptive response to stressors or adverse threats. Stressors can be psychological, physical, real, or perceived. Anxiety, sadness, depression, overwhelm, excitement, fear and anger are all common stressors that can affect the gastrointestinal tract. Lifestyle stressors can also impact your health. These include time management, inadequate sleep, changes in the environment, work or relationship issues, watching the news, and much more.
Stress is the body’s natural hormonal response to dealing with a situation. It can be harmful to your physical and mental health when there is prolonged exposure to stressors, such as experiencing a traumatic event. The physical reactions to stress include increased heart rate and perspiration.
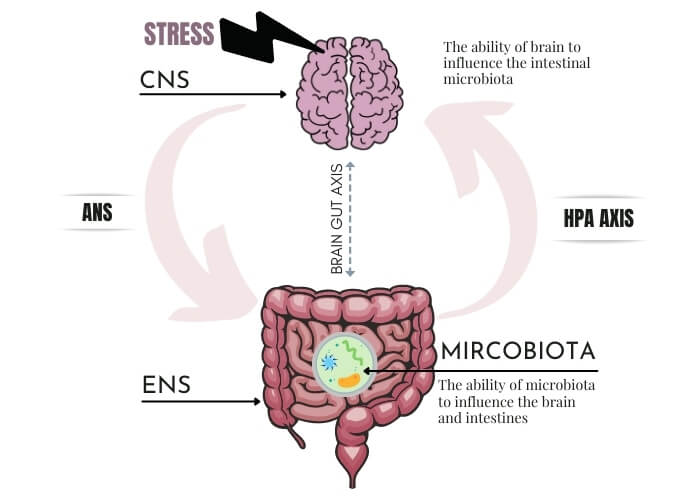
What is the connection between stress and inflammatory bowel disease?
There is a two-way influence between stress and IBD. Inflammation leading to symptoms, such as pain, can lead to stress. And whenever stress occurs, the development of IBD symptoms can be affected to some extent. Stress associated with adverse life events or chronic psychological stress has been shown to be associated with subclinical (unrecognizable) increases in inflammation.
Multiple pathways, including the autonomic nervous system and hypothalamic-pituitary-adrenal axis (HPA axis), are activated when the brain receives stress input. Because there is a two-way connection between the brain and nerves in the lining of the gut (brain-gut axis), stress will eventually affect the contractions and movements of the gastrointestinal tract. This increases gut sensitivity and causes bacteria to cross the gut lining and activate the immune system, increase inflammation in the gut, and change the gut microbiota.
Gut microbiota, or microbiome, is a micro-system of organisms in the gut. This microbiome consists of bacteria, viruses, fungi, and parasites. There are two kinds of microbes: beneficial and pathogenic organisms. Beneficial organisms have a mutually beneficial relationship with our bodies. They help prevent bowel disorders, cancer, and chronic diseases. Pathogenic organisms have the propensity to cause diseases if left unchecked. In a healthy person, these two kinds of organisms live peacefully. Disruption of this peaceful existence and increase in the pathogenic organisms can occur with illnesses, medications, and certain diets.
There is strong evidence that gut microbiota (microbes that reside in the gut) has an important role in the interactions between gut and brain. The trillions of microorganisms that live in the human gut may also affect behavior and emotions. In inflammatory bowel disease, alteration of the gut microbiota causes a reduction in beneficial organisms.
Common emotional disorders among people with inflammatory bowel disease include depression, anxiety, and perceived stress.
How do I deal with stress with inflammatory bowel disease?
Life is a balance, and so is IBD. Getting this balance right takes time and effort. Listen to your body and adapt to activities that you enjoy doing.
Ways to manage stress effectively include:
- Strike a better balance between your work and lifestyle. You can organize your work schedule to be similar every day and schedule breaks between activities.
- Identify your key stressors. Identify situations that exceed your ability to cope. Of course, some problems can’t be avoided. Planning ahead, rearranging your environment, and managing things that you can control can help you cope better during stressful situations. If coping with symptoms is the primary cause of your stress or if you feel depressed or anxious, talk to your healthcare team. They may recommend and help you connect with a psychiatrist or prescribe appropriate treatment.
- Use constructive self-talk. Address the ongoing commentary in your mind. If there are persisting negative thoughts, replace them with constructive self-talk, letting go of the past and moving forward focusing with new possibilities.
- Socialize or spend time with family and friends. People with IBD tend to isolate and become lonely due to a fear of experiencing symptoms in social situations or public places. For social situations, plan ahead for managing episodes of diarrhea or abdominal pain. Identify bathroom locations where you will be and carry extra supplies you may need. Mobile apps can assist you in locating nearby restrooms within the U.S. and around the world.
Sharing your concerns with your family and friends can provide much-needed support. In addition, you can connect with Crohn’s and Colitis communities and their members who have similar experiences.

Focus on self-care as a lifestyle requirement
There are many aspects of self-care that can help you cope in the short- and long term. These include:
- Exercising and sports
- Deep breathing
- Mediation and yoga
- Listening to relaxing music
Activities, such as creative projects, gardening, or spending time in nature, can similarly add to feelings of enjoyment and inner peace. Overall, add daily activities to your schedule that you enjoy and that lift your spirit. As important, take time to rest and get the right amount of quality sleep your body needs.
Feed your body with healthy nutrition
Adapt to a diet that builds a healthy gut microbiome. Aim to balance your intake of foods and beverages that are good for you with those that may worsen your symptoms. Work with a dietician to evaluate foods and beverages, keep a diary of your foods and symptoms on your KnowYourMeds app, and find the balance that works for you. You might discover that a plant-based, minimally processed and high-fiber diet is beneficial to your gut microbiome and symptoms.
Maintain a positive and optimistic mindset
There are many things beyond our control. Keeping a positive attitude can help offset difficult situations and your reactions to them. Stress comes from how you respond to a stressor. Refocus your mind on doing things that make you happy and more relaxed. Even changing your focus from negative to positive thoughts or feelings can provide immediate relief from stress.


